Abstract
Background/Objective:
The aim of the study was to compare the prevalence of undernutrition in children on presentation to hospital and on discharge.
Methods:
On a screening week, 141 children aged from birth to 17 years who were hospitalised for ⩾72 h were reviewed on presentation and discharge or after 3 months (if still in hospital) by auditing hospital records. Weight for age standard deviation (s.d.<−2) was used to define undernutrition on admission and discharge. The number of children referred for dietetic advice was recorded.
Results:
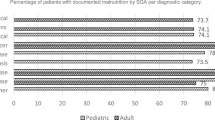
The prevalence of undernutrition on admission was 27% (14% moderate (s.d.: −2 to −3) and 13% severe (s.d.: ⩾−3)) according to weight s.d. and increased to 32% by discharge (11% moderate; 21% severe). The most nutritionally vulnerable children, with a prevalence of undernutrition from 33 to 53% on admission, were aged less than 2 years, inpatients for >1 month and those with multiple medical problems. In all, 74% (n=104) of cases were referred to Dietetics, including 73% (n=79) of those without evidence of undernutrition.
Conclusions:
Undernutrition is a major problem in children during hospitalisation. The risk of nutritional depletion needs to be identified at the time of admission, especially for children under 2 years and those with multiple medical problems, in order to initiate appropriate nutritional intervention.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Joosten KF, Hulst JM . Prevalence of malnutrition in paediatric hospital patients. Curr Opin Pediatr 2008; 20: 590–596.
Pawellek I, Dokoupil K, Koletzko B . Prevalence of malnutrition in paediatric hospital patients. Clin Nutr 2008; 27: 72–76.
Marteletti O, Caldari D, Guimber D, Mention K, Michaud L, Gottrand F . Malnutrition screening in hospitalized children: influence of the hospital unit on its management. Arch Pediatr 2005; 12: 1226–1231.
Dogan Y, Erkan T, Yalvaç S, Altay S, Cokuğraş FC, Aydin A et al. Nutritional status of patients hospitalized in paediatric clinic. Turk J Gastroenterol 2005; 16: 212–216.
Ozturk Y, Buyukgebiz B, Arslan N, Ellidokuz H . Effects of hospital stay on nutritional anthropometric data in Turkish children. J Trop Pediatr 2003; 49: 189–190.
Hankard R, Bloch J, Martin P, Randrianasolo H, Bannier MF, Machinot S et al. Nutritional status and risk in hospitalized children. Arch Pediatr 2001; 8: 1203–1208.
Hendrikse W, Reilly JJ, Weaver LH . Malnutrition in a children’s hospital. Clin Nutr 1997; 16: 13–18.
Hendricks KM, Duggan C, Gallagher L, Carlin AC, Richardson DS, Collier SB et al. Malnutrition in hospitalized paediatric patients. Current prevalence. Arch Pediatr Adolesc Med 1995; 149: 1118–1122.
Moy RJD, Smallman S, Booth IW . Malnutrition in a UK children’s hospital. J Hum Nutr Diet 1990; 3: 93–100.
Rocha GA, Rocha EJ, Martins CV . The effects of hospitalization on the nutritional status of children. J Pediatr (Rio J) 2006; 82: 70–74.
Merritt RJ, Sinatra FR, Smith GA . Nutritional support of the hospitalized child. Adv Nutr Res 1983; 5: 77–103.
Hulst JM, Zwart H, Hop WC, Joosten KF . Dutch national survey to test the STRONGkids nutritional risk screening tool in hospitalized children. Clin Nutr 2010; 29: 106–111.
Sermet-Gaudelus I, Poisson-Salomon AS, Colomb V, Brusset MC, Mosser F, Berrier F et al. Simple pediatric nutritional risk score to identify children at risk of malnutrition. Am J Clin Nutr 2000; 72: 64–70.
Campanozzi A, Russo M, Catucci A, Rutigliano I, Canestrino G, Giardino I et al. Hospital-acquired malnutrition in children with mild clinical conditions. Nutrition 2009; 25: 540–547.
De Moraes Silveira CR, De Mello ED . Antonacci Carvalho PR. Evolution of nutritional status of paediatric in patients of a tertiary care general hospital in Brazil. Nutr Hosp 2008; 23: 599–606.
Child Growth Foundation. Four-in-one growth charts. UK cross-sectional reference data: 1996-0/1. Available from Child Growth Foundation, London, UK.
Cole TJ, Freeman JV, Preece MA . British 1990 growth reference centiles for weight, height, body mass index and head circumference fitted by maximum penalized likelihood. Stat Med 1998; 17: 407–429.
Cole TJ, Green PJ . Smoothing reference centile curves: the LMS method and penalized likelihood. Stat Med 1992; 11: 1305–1319.
WHO. Physical status: the use and interpretation of anthropometry. WHO Technical Report Series, 854. WHO: Geneva, 1995.
Cole TJ, Freeman JV, Preece MA . Body mass index reference curves for the UK, 1990. Arch Dis Child 1995; 73: 25–29.
Ungar WJ . Challenges in Health State Valuation in Paediatric Economic Evaluation: Are QALYs Contraindicated? Pharmacoeconomics 2011; 29: 641–652.
O' Brien I, Duffy A, Nicholl H . Impact of childhood chronic illnesses on siblings: a literature review. Br J Nurs 2009; 18, 1358 1360–1365.
Hopia H, Tomlinson PS, Paavilainen E, Astedt-Kurki P . Child in hospital: family experiences and expectations of how nurses can promote family health. J Clin Nurs 2005; 14: 212–222.
Afzal NA, Addai S, Fagbemi A, Fagbemi A, Murch S, Thomson M, Heuschkel R . Refeeding syndrome with enteral nutrition in children: a case report, literature review and clinical guidelines. Clin Nutr 2002; 21: 515–520.
Children’s Nutrition Survey 2011, University of Ulster, cns@ulster.ac.uk.
Sneve J, Kattelmann K, Ren C et al. Implementation of a multidisciplinary team that includes a registered dietitian in a neonatal intensive care unit improved nutrition outcomes. Nutr Clin Pract 2008; 23: 630–634.
Koletzko B, Goulet O, Hunt J et al. Guidelines on paediatric parenteral nutrition of the European Society of Paediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) and the European Society for Clinical Nutrition and Metabolism (ESPEN), supported by the European Society of Paediatric Research (ESPR). J Paediatr Gastroenterol Nutr 2005; 41: S1–S4.
Acknowledgements
We would like to thank all the members of the multi-disciplinary teams caring for these patients while in hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Contributors: The study was designed by Dr Susan Hill, Vanessa Shaw and Prof. Alan Lucas. The subjects were recruited by Dr Judith Pichler. Data collection and analyses were done by Dr Judith Pichler and Prof. Alan Lucas. The manuscript was written by Dr Judith Pichler with the provision of significant advice and consultation by all other authors. All authors critically appraised the manuscript.
Rights and permissions
About this article
Cite this article
Pichler, J., Hill, S., Shaw, V. et al. Prevalence of undernutrition during hospitalisation in a children’s hospital: what happens during admission?. Eur J Clin Nutr 68, 730–735 (2014). https://doi.org/10.1038/ejcn.2014.21
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2014.21
This article is cited by
-
Hospital-acquired malnutrition in paediatric patients: a multicentre trial focusing on prevalence, risk factors, and impact on clinical outcomes
European Journal of Pediatrics (2021)