Article Text
Abstract
Objectives To assess the effectiveness of thermostatic mixing valves (TMVs) in reducing bath hot tap water temperature, assess acceptability of TMVs to families and impact on bath time safety practices.
Design Pragmatic parallel arm randomised controlled trial.
Setting A social housing organisation in Glasgow, Scotland, UK.
Participants 124 families with at least one child under 5 years.
Intervention A TMV fitted by a qualified plumber and educational leaflets before and at the time of TMV fitting.
Main outcome measures Bath hot tap water temperature at 3-month and 12-month post-intervention or randomisation, acceptability, problems with TMVs and bath time safety practices.
Results Intervention arm families had a significantly lower bath hot water temperature at 3-month and 12-month follow-up than families in the control arm (3 months: intervention arm median 45.0°C, control arm median 56.0°C, difference between medians, −11.0, 95% CI −14.3 to −7.7); 12 months: intervention arm median 46.0°C, control arm median 55.0°C, difference between medians −9.0, 95% CI −11.8 to −6.2) They were significantly more likely to be happy or very happy with their bath hot water temperature (RR 1.43, 95% CI 1.05 to 1.93), significantly less likely to report the temperature as being too hot (RR 0.33, 95% CI 0.16 to 0.68) and significantly less likely to report checking the temperature of every bath (RR 0.84, 95% CI 0.73 to 0.97). Seven (15%) intervention arm families reported problems with their TMV.
Conclusions TMVs and accompanying educational leaflets are effective at reducing bath hot tap water temperatures in the short and longer term and are acceptable to families. Housing providers should consider fitting TMVs in their properties and legislators should consider mandating their use in refurbishments as well as in new builds.
Statistics from Altmetric.com
Introduction
Approximately 2000 emergency department attendances and 500 hospital admissions following bath water scalds to children occur in the UK each year.1 Admissions mostly occur in children aged under 5 years, often involving prolonged inpatient stays, transfer to a specialist hospital or burns unit.1 The cost of treating a severe scald has been estimated at £250<TS, thin space here>000.1 Longer-term effects include disability, disfigurement or psychological harm.
What is already known on this topic
▶ Hot bath water scalds are an important public health problem; their incidence has not declined over recent years.
▶ Thermostatic mixing valves (TMVs) have the potential to reduce scald risk but there have been no randomised controlled trials assessing their effectiveness and acceptability to families.
What this study adds
▶ TMVs and educational leaflets are effective in reducing bath hot tap water temperature in the short and longer term and are acceptable to families.
▶ Families with TMVs are less likely to check bath water temperature. The importance of checking temperature should be emphasised during TMV fitting and further research should explore ways of increasing such safety practices.
Children from disadvantaged areas2 and younger children are at greater risk of scalds.3 Commonly bath water scalds happen when children fall or climb unsupervised into water; a child turns on the hot tap or a parent puts a child into water that is too hot.1 4 Home water thermostats are frequently set at 60°C or above.5 Water at this temperature can cause a full thickness burn in an adult in 5 seconds,1 and more quickly in children.6 It is recommended that the bath hot tap water temperature should not exceed 46°C.7
Early studies offering educational interventions to promote tap water temperature testing and/or thermostat reduction demonstrated at best a small effect on tap water temperatures, often reducing them insufficiently to reduce the risk of scalds 8,–,11 A recent meta-analysis of home safety interventions, most of which comprised education and providing equipment to prevent a range of childhood home injuries, found a significant reduction in water temperatures; but again, in most studies the temperature post-intervention remained above current recommended levels.12 Legislation to reduce thermostat settings has been more successful with uncontrolled studies demonstrating reductions in hospital admission rates, total body area burnt, scarring and skin grafting.13
Thermostatic mixing valves (TMVs) are designed to reduce the risk of scalding from hot tap water. They do not affect the temperature of stored hot water or interfere with heating systems and allow hotter water to be supplied to different sites within the home. They fit across bath hot and cold water supply pipes and set the hot tap water at a fixed temperature, regardless of changes in pressure or temperature in the water supply system. As the bath water supply pipes are usually housed behind bath panels, they are not easily accessible by families. Although families could theoretically adjust their TMV, its positioning would make this difficult. The English government recently announced amendments to building regulations requiring TMVs to be fitted in new build properties, extensions and buildings converted to dwellings.14 However, TMVs have not been tested for effectiveness and acceptability in the domestic setting in the UK, and importantly effectiveness has not been tested in a high-risk population. We have therefore conducted a randomised controlled trial in deprived communities in Glasgow.15 16
Methods
Design
Pragmatic (ie, designed to measure the benefit of the intervention in normal practice) parallel arm randomised controlled trial.
Participants
Generalisabilty was maximised using broad inclusion and minimal exclusion criteria.
Families with children under 5 years living in Glasgow Housing Association (GHA) housing (Europe's largest social housing provider) were eligible for inclusion. Exclusion criteria were moving from the property, pipe work unsuitable for TMV fitting and participation in other tap water scald prevention projects.
Recruitment was by written invitation from GHA to tenants on the East End Child Safety Project database, which is a database of families who have taken part in a previous child safety project and to tenants aged 18–40 years identified from the GHA tenant database; or by face-to-face contact with local housing organisations. Families were randomised to intervention or control arms. The intervention comprised:
▶ A study specific educational leaflet mailed before TMV fitting, providing information on how bath water scalds happen, the time taken for scalds to occur at different temperatures, usual bathing temperatures, what a TMV is and a true story of a 2-year-old child scalded from hot bath water.
▶ A TMV set at a maximum temperature of 45°C fitted by a qualified plumber from City Building (Glasgow) limited liability partnership (LLP). Fitting usually involved removing the bath panel, connecting the TMV to hot and cold water supply pipes and replacing the bath panel; and
▶ A waterproof guide was hung on the tap by the plumber. This provided information about running a bath with a TMV fitted, reiterated some information on the leaflet and advice to continue checking the temperature of bath water and not to leave children alone in the bath.
Families randomised to the control arm were offered the intervention after collection of follow-up data.
Objectives
The objectives were to assess the effectiveness of TMVs in reducing bath hot tap water temperature; acceptability of TMVs to families and impact on bath time safety practices.
Definition of primary and secondary outcome measures
The primary outcome measure was bath hot tap water temperature at 3-month and 12-month post-TMV fitting (intervention arm) or post-randomisation (control arm) considered to be the outcome of most interest to policymakers. Secondary outcomes for the intervention arm included TMV problems (eg, failures, replacements), adjustment of TMV settings and satisfaction with TMVs and fitting process. Secondary outcomes for both arms included bath hot tap water temperature ≤46°C, satisfaction with bath hot tap water and bath time safety practices, chosen to reflect relevance to housing providers, families with young children and policymakers. They were measured 12-month post-TMV fitting and 12-month post-randomisation
Baseline data
Baseline data, collected by postal or telephone questionnaire, included sociodemographic and economic characteristics, bath time safety practices and satisfaction with hot water supply. Families were offered incentives (free bath mat or first aid kit) to increase response rates for the baseline questionnaire.17 GHA reported that accessing the homes of their tenants was difficult, often requiring multiple attempts. In view of this, families were offered a £10 gift voucher for use in local stores on completion of a water temperature measurement and we planned to ask participants to only have one water temperature measurement during the study, with the first 50% recruited to each arm selected for baseline measurements. A qualified plumber from City Building (Glasgow) LLP measured temperatures using a Type K thermocouple thermometer and rounded immersion probe. The bathroom sink hot water temperature was also measured to detect other methods of reducing water temperature—for example, reducing thermostat settings.
Follow-up data
Primary outcome measure
Families who had not been selected for a baseline temperature measurement were randomly assigned, by treatment arm, to 3-month or 12-month water temperature measurements, using a random number list.18 Where plumbers repeatedly visited homes but were unable to find anyone at home (hereafter referred to as unable to access property), families who had had a baseline measurement were selected at random for a follow-up temperature measurement, until measurements were obtained on at least 15 families, at each follow-up time point, in each arm. Families were offered a £10 gift voucher for use in local stores on completion of a water temperature measurement.
Secondary outcome measures
Data were collected by postal or telephone questionnaire and a £5 gift voucher was offered to families on completion of the follow-up questionnaire to increase response rates. Problems with TMVs were also ascertained from repair requests or complaints made to GHA.
Sample size
Ten families per arm were required to detect a reduction in the mean bath hot tap water temperature from 60.4°C (SD 9.1°C)19 in the control arm to the recommended temperature of 46°C 20 in the intervention arm (90% power, two-sided 5% significance level). However, baseline measurements indicated a larger SD than this in the control arm (mean 60.8°C, SD 10.25°C) and temperatures immediately after valve fitting were not normally distributed with a very small SD (mean 45.5°C, SD 0.51°C). The sample size was therefore recalculated based on reducing mean temperature from 60.8°C to 46°C (SD 10.25°C), (90% power, two-sided 5% significance level), assuming the asymptotic relative efficiency of the Mann-Whitney U test relative to the t test is never lower than 0.864.21 Under these assumptions 14 families per arm were required. Random sampling continued until measurements were achieved from 15 families in each arm at 3 months and 12 months.
For secondary outcome measures, 50 families per arm provided 80% power at the 5% significance level (two-sided) to detect a difference in the proportion of families satisfied with their water temperature from 90% in the control arm to 67% in the intervention arm. Fifty families in the intervention arm provided 80% power (one-sided 5% significance) to test the hypothesis that the proportion of TMVs removed, disabled or adjusted did not exceed 6.5% if the true proportion removed, disabled or adjusted was 1%. To allow for losses to follow-up, recruitment aimed for a total of 120 participants.
Randomisation
The trial statistician used Stata22 to generate the randomisation schedule with a permuted block design and random block size. Equal numbers of consenting families were allocated to arms. No stratification was used. Allocations were placed in sequentially numbered, opaque, sealed envelopes, which were opened by an independent researcher.
Blinding
It was not possible to blind participants, plumbers or researchers to treatment arm allocation. The analysis was undertaken blind to allocation, but the analyst correctly guessed allocation for 100% and 84% of cases at 3 months and 12 months, respectively.
Withdrawals
Participants were free to withdraw from the trial at any stage. Data were included in the analyses up to the point of withdrawal.
Statistical methods
Data were double entered into an Access database with discrepancies identified and corrected. Conforming to a prespecified analysis plan, participants were analysed in the group they were randomised to regardless of the intervention received. Bath hot tap water temperatures were described using medians and IQR. The primary analysis compared temperatures between treatment arms using the Mann-Whitney U test and estimated the difference between median values and 95% CI around the difference using the Bonett-Price CI method. These analyses were based on families with follow-up temperature measurements. Two sensitivity analyses were undertaken. First, where families had missing follow-up temperatures, we assumed there had been no change from baseline and follow-up temperatures were replaced with the baseline temperature for that family, or where baseline temperatures were unavailable, with the median baseline temperature for that treatment arm. Second, as the potential for temperature reduction depended on the baseline temperature, we adjusted for baseline temperatures (or median treatment arm temperature if baseline temperature was missing) by calculating change scores.
Secondary outcomes were compared between treatment arms by estimating relative risks and 95% CI. Where the prevalence of outcomes at baseline differed between treatment arms by more than 10%, we estimated the Mantel-Haenszel adjusted relative risk and 95% CI.
Ethical and organisational approval
Ethics committee review was undertaken by Nottingham 1 NHS Research Ethics Committee. Organisational approval was gained from NHS Nottinghamshire County
Results
Participant flow and follow-up
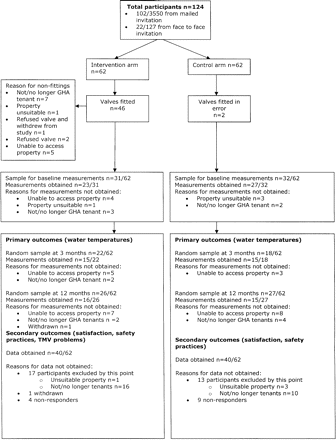
The flow of participants is shown in figure 1. In all, 124 participants were randomised. Data on participants excluded after randomisation and collection of baseline data on those who withdrew are included in the analysis of baseline data.23 Losses to follow-up and the reasons for loss to follow-up are given in figure 1.
Flow of participants through trial. GHA, Glasgow Housing Association.
Baseline questionnaire data were collected between June 2006 and January 2007, with TMV fitting and temperature measurements undertaken between July 2006 and February 2007. The median time between recruitment and baseline temperature measurement was 59.5 days in the intervention arm and 48 days in the control arm. Three-month temperatures were collected between February and April 2007, follow-up questionnaire data between August 2007 and April 2008 and 12-month temperatures between November 2007 and April 2008. The median time between TMV fitting and 12-month temperature measurement in the intervention arm was 467 days and between randomisation and 12-month temperature measurement in the control arm was 449 days.
Analysis
Participants' characteristics are shown in table 1 and baseline description of hot water temperature, satisfaction and bath time safety practices in table 2. Control arm participants were more likely to live in single adult households and run baths using cold water first and less likely to have left children alone in the bath or bathroom while the bath was running. The median bath hot tap water temperature in the intervention arm at baseline was 55°C (IQR 54–58°C) and 58°C (IQR 55–62°C) in the control arm. Most families were happy with their bath hot water temperature and described it as very hot. All those unhappy with the temperature, described it as hot/very hot. Water temperatures, the infrequent use of cold water first when running the bath and the number of families leaving children alone in the bath or bathroom suggests a considerable proportion of families were at risk of scalds.
Characteristics of participants at baseline, by treatment arm (%)
Bath hot tap water temperature, satisfaction with water temperature and bath time safety practices at baseline, by treatment arm (% unless specified)
Figure 2 shows the distribution of bath hot tap water temperatures in the two groups at baseline, and at 3 months and 12 months. Table 3 shows that at both follow-up time points during follow-up, bath hot tap water temperatures were significantly lower in the intervention than in the control arm. Findings were robust to adjusting for baseline tap water temperature and to replacing missing temperatures with baseline values. There was no significant difference in bathroom sink hot tap water temperatures between arms at either time point. Table 4 shows that at 12-month follow-up intervention arm families were significantly more likely than control arm families to have a bath hot tap water temperature of 46°C or below and be satisfied with the temperature. They were significantly less likely to report their bath hot tap water as being too hot and to check the bath water temperature for every bath.
Box plot showing the distribution of bath hot tap water temperatures by treatment group at baseline, 3-month and 12-month follow-up. The bottom and top of the boxes represent the 25th and 75th percentiles, the line in the box is the median. The lines drawn from the box indicate the range, and outlying values are indicated separately.
Primary outcome measures at 3-month and 12-month follow-up by treatment arm
Secondary outcome measures at 12-month follow-up by treatment arm (percentage)
Few families were unhappy with their bath hot tap water temperature at 12-month follow-up (nine (23%) in the control arm and five (13%) in the intervention arm). The majority of those that were unhappy (n=10) reported that the temperature was hot or very hot, with only two reporting it was not warm enough. However, secondary outcomes measured only in the intervention arm (table 5) showed that 12 (36%) families agreed or strongly agreed that their bath water wasn't hot enough and nine (27%) that they could not top up the bath with hot water while in the bath. The majority of families in the intervention arm with a TMV were satisfied with the valve and the fitting process and would recommend TMVs to a friend. Seven of the 46 families (15%) who had TMVs fitted had problems with their TMV; four families reported a low water pressure post-TMV fitting, and in three of these cases the problem was not found to be related to the TMV. One TMV was replaced because of malfunctioning, one family reported a leak after installation and one family reported no hot water from their hot bath tap and the valve was cleaned.
Satisfaction with the TMV and fitting process at 12-month follow-up
Families who did not have any follow-up water measurements either because their properties could not be accessed or because they had been excluded did not differ significantly on any baseline characteristics from those who did have follow-up hot water measurements. Compared to those lost to follow-up, families who completed the follow-up questionnaire were significantly more likely to be happy with their bath hot water temperature (70% vs 45%, difference between percentages (25%, 95% CI 7% to 42%) and their water flow at baseline (50% vs 30%, difference between percentages 20%, 95% CI 3% to 38%) and significantly less likely to be receiving state benefits (81% vs 95%, difference between percentages −14%, 95% CI −25% to −4%)
Discussion
Principal findings
TMVs fitted in the homes of families in disadvantaged communities and accompanying educational leaflets are effective in reducing bath hot tap water temperature to the current recommended ‘safe’ level for at least 12 months post-installation. Most families were satisfied with the temperature and speed of flow of their hot bath water after fitting, and with the fitting process. Those with a TMV were significantly less likely to check the bath temperature of every bath, but we did not find a negative effect on other safety practices.
Strengths and weaknesses of the trial
As the first randomised controlled trial to assess the effectiveness of TMVs and accompanying educational leaflets in a severely disadvantaged population, with a small proportion of families from minority ethnic groups our findings should be generalisable to similar communities in the UK. Generalising our findings to all families with young children in social housing should be undertaken with caution as it has not been possible for us to estimate our recruitment rate among families with young children owing to a lack of information on households containing children in GHA records. Furthermore, our findings may not be generalisable to families who are required to pay the costs of TMV fitting. We also cannot assume that the levels of uptake of TMVs, satisfaction and problems with TMVs found in our trial would necessarily be replicated in the wider population. Furthermore, our trial was undertaken with one large social housing provider having potentially greater access to resources, skills and economies of scale. Smaller housing providers may find implementing TMVs more difficult.
Just over 25% of participants were lost to follow-up, mainly as a result of household moves. However, high follow-up questionnaire response rates and the required number of follow-up temperature measurements were achieved and sensitivity analyses suggest findings for the primary outcome are unlikely to be biased by losses to follow-up. Those lost to follow-up for secondary outcome measures were significantly less happy with their bathwater temperature and water flow at baseline than those continuing in the trial, hence satisfaction with hot water temperature and water flow at follow-up may have been lower than we have reported, in both treatment arms.
As with many public health interventions it was not possible to blind participants and plumbers to treatment arm allocation. Additionally, the analyst was able to correctly guess the treatment arm allocation for most participants for the primary outcome, effectively unblinding the analysis.
Our trial was not adequately powered to detect a reduction in the incidence of bath tap water scalds, and a very much larger trial would be required to do this. However, we have shown that TMVs are effective at maintaining a bath hot tap water temperature at or below 46°C, and water at this temperature would take more than 9 minutes to cause a partial thickness burn,6 hence temperature is likely to be a good proxy measure for bath tap water scalds.
Comparisons with previous research
We found higher levels of satisfaction with TMVs than a previous study, possibly because 95% of valves in the earlier study failed.24 We are not aware of any published studies reporting the impact of TMV fitting on bath time safety practices.
Implications for injury prevention practice and further research
Our trial demonstrated that TMVs and accompanying educational leaflets are effective in reducing bath hot tap water temperatures and are acceptable to families. TMVs may benefit a wider population than that used in our trial, especially older people and those with disabilities. The current amendment to English building regulations which relate to new build homes or major refurbishments such as adding a bathroom as part of an extension is likely to protect a small proportion of the population and to disproportionately protect more affluent members of the community, potentially widening inequalities in thermal injuries. Housing providers should consider fitting TMVs in their properties and legislators should consider requiring the fitting of TMVs as part of bathroom refurbishments, such as those installing new baths, which may not be covered by the current amendments to building regulations. We did not find the educational leaflets used as part of the intervention improved bath time safety practices, and the intervention group were less likely to test bath water temperature at follow-up than control families. Further research is needed to explore ways of improving bath time safety practices. TMVs have an in-built safety mechanism to cut off the flow of hot water to prevent scalding in the event of a disruption to the cold water supply. Hence, even if families are less likely to test bath water temperature, this should only increase the risk of a scald if there is a simultaneous disruption to the cold water supply and the TMV malfunctions.
As always, the limitations of a single trial must be borne in mind when considering wider scale implementation of its findings. Wider scale implementation should be accompanied by surveillance and monitoring, including programme components; TMV uptake; tap water temperatures over a longer time period; satisfaction, acceptability and TMV problems; maintenance requirements and impact on other bath time safety practices. Experience with other injury prevention initiatives suggests a range of promotional activities such as media campaigns, incentives and education can be beneficial before implementing legislation.25 A similar approach may be needed for successful wide scale implementation of TMVs. Finally, cost is a frequently cited argument against fitting TMVs,26 and we are conducting an economic evaluation of this trial and findings will be presented elsewhere.
Acknowledgments
The authors thank the study participants, East End Child Safety Project workers for their advice on questionnaire design and help with recruiting participants; Professor David Stone, University of Glasgow, for his support throughout the project and comments on the paper for submission; PACT team (Parents and Children Together) for help with recruiting participants; Jim Sodden, of the GHA for facilitation of the study within GHA; Angela McMurran, Bob McGuire, Charlie Thomas, Janet McDonald, Jannette Rawls, Linda Neil of the Local Housing Organisations for facilitating the study within their locality; Alan Skimins and the plumbers of City Building LLP (Glasgow) for coordination and fitting of TMVs, tap water measurements and liaison with Glasgow Housing Association Central Repairs team; Michelle Hubbard and Rose Clacy, members of the Consumer Research Advisory Group at Nottinghamshire County Teaching PCT for development of the study invitation letter and information leaflet; Angus Horne of Horne Engineering for advice and demonstration of the workings of TMVs; Brian Hancock and John Slater, Nottinghamshire County Teaching PCT, for design of the bath tap hanger and study information leaflet; Mark Stevenson of The Scottish Burned Children's Club for facilitating access to a parent of a child with a bathwater scald injury and to the parent for providing the real life story for the study information leaflet.
References
Footnotes
-
Funding National Institute for Health Research, Accidental Injury Prevention Research Initiative (001/0009). The final study design, data collection and analysis, interpretation of results and paper writing was the sole responsibility of the authors. The views and opinions expressed in this paper do not necessarily reflect those of the funding body.
-
Competing interests MH is an employee of the Child Accident Prevention Trust (CAPT) which is a registered charity. ‘INTA’ a TMV manufacturer has previously sponsored a CAPT publication. There is the possibility that CAPT could benefit in the future by gaining sponsorship for other publications from TMV manufacturers.
-
Ethics approval Nottingham 1 NHS research ethics committee (reference number 05/Q2403/37)
-
Provenance and peer review Not commissioned; externally peer reviewed.