Article Text
Abstract
Background Conflict in healthcare is a well-recognised but under-examined phenomenon. Little is known about the prevalence and causes of conflict across paediatric specialties.
Objective To report the frequency and characteristics of conflict in a paediatric hospital.
Design and setting An explanatory sequential mixed-method approach was adopted. A bespoke questionnaire recorded frequency, severity, cause and staff involved in conflict prospectively. Data were recorded for the same two 12-week periods in 2013 and 2014, in one UK children's teaching hospital. Data were analysed using descriptive statistics and correlation, the findings of which informed the construction of a semistructured interview schedule. Qualitative interviews were conducted with six key informant healthcare professionals to aid data interpretation; interviews were analysed thematically.
Results 136 individual episodes of conflict were reported. The three most common causes were ‘communication breakdown’, ‘disagreements about treatment’ and ‘unrealistic expectations’. Over 448 h of healthcare professional time was taken up by these conflicts; most often staff nurses, consultants, doctors in training and matrons. The mean severity rating was 4.9 out of 10. Qualitative interviews revealed consensus regarding whether conflicts were ranked as low, medium or high severity, and explanations regarding why neurology recorded the highest number of conflicts in the observed period.
Conclusions Conflict is prevalent across paediatric specialties, and particularly in neurology, general paediatrics and neonatology. Considerable staff time is taken in managing conflict, indicating a need to focus resources on supporting staff to resolve conflict, notably managing communication breakdown.
- Paediatric Practice
- Health services research
This is an Open Access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/
Statistics from Altmetric.com
What is already known on this topic
Despite some empirical research documenting conflict in paediatric intensive care units, it remains an under-researched phenomenon.
Communication is often identified as a significant contributor to conflict.
What this study adds
Staff nurses and consultants are the practitioners most heavily involved in managing conflict.
Conflict has a substantial toll on staff time, and particularly so within neurological settings.
Training in conflict management, focused on communication skills, should be offered to front-line staff.
Introduction
Despite conflict being a well-recognised facet of healthcare, it remains an under-researched phenomenon. The incidence and prevalence of conflict has been the focus of a small number of empirical studies. An observational study of an adult intensive care unit (ICU) reported conflicts occurring at a rate of 26.6% in a retrospective study of 7400 staff account for the previous week of practice.1 This contrasts with a prospective interview study which reported conflict in 48% of 102 ICU cases,2 with the majority of conflict arising over decisions around the provision of life-sustaining treatment.2 A study of parents’ experiences of conflict in a paediatric ICU (PICU) identified that nearly half of their sample of 110 families reported conflict.3 Conflicts in adult ICU and PICU have considerable similarities, despite their very different patient groups and case mixes.3
ICUs provide a ripe environment for conflict, with a mixture of very sick patients, high mortality, multiple specialties and a frequent need for urgent decisions on complex matters.4 In paediatrics, a shared model of decision-making is the norm.5 However, the multipartner nature of medical encounters (such as the triad dynamic of clinicians, patient and relatives) may increase the complexity of cases and therefore the potential for disagreement and conflict.6 In end-of-life decision-making for children, the majority of relatives report that the decision to withdraw care should be made jointly between clinicians and families,7 with a small number believing the decision lies solely with the families.8 The input the child has into the decision-making process depends upon the individual's level of maturity as assessed by the clinician.9
Limited work has been conducted outside of the ICU context examining the incidence and severity of conflict in paediatric settings, though some papers offer reflexive accounts from practitioners around conflict,10 case reviews and court reports,11 tracing the history of care standards over treatment decision-making over time12 and mapping how conflict escalates.13
Across adult and paediatric services, communication difficulties are identified as a significant contributor to conflict,14–17 as are cross-cultural difficulties18 and religious beliefs.19 Other studies have suggested that conflict may arise when relatives are not fully supported to understand treatment and care decisions.20 Underpinning each of these causes can be different understandings of the clinical situation21 and different interpretations of futility22 and likely prognosis.11
Thus, while there is a small evidence base examining the causes, incidence and sequelae of conflict, quantitative studies have been located in the ICU rather than across specialties, and other publications have been reflexive accounts rather than research question-driven empirical investigations. This study sought to document, for the first time, the frequency, severity and attributed causes of conflict between families/patients and staff across specialties in a UK paediatric hospital.
Methods
An explanatory sequential mixed-method approach was adopted.23 A bespoke questionnaire was designed to capture the frequency, severity, cause of conflict, staff involved and time taken in managing the conflict. The data were collected prospectively for the same two 12-week periods in 2013 and 2014, at the Evelina London Children's Hospital. The same quarter was used each year to control for seasonal fluctuations in case mix and bed occupancy. Senior staff in each ward of the hospital were identified to report conflict on a weekly basis; weekly reminders were issued to minimise missing data.
Descriptive data are presented with averages and ranges for frequency, severity, cause of conflict, staff involved and length of involvement in conflict reported. Spearman rank order coefficients were also run to determine whether there were associations between variables; significance was set at p<0.05. The findings of the questionnaire phase informed the construction of a qualitative interview schedule.
Qualitative interviews were conducted with key informant healthcare professionals to aid data interpretation. Interviewees were sampled from the cohort of staff in wards where conflict had been identified as frequent and/or severe and who had personal experience of conflict with patients/parents. Data collection ceased at saturation,24 at which point six interviews had been conducted (one senior nurse, two consultants, one doctor in training and two staff nurses). Iterative thematic analysis was conducted,25 proceeding through a five-stage process of familiarisation, identifying a thematic framework, indexing the data, synthesising across respondents and data interpretation to form key themes.
The study is part of a wider piece of evaluation work and consequently did not require National Health Service ethical approvals.
Results
One hundred and thirty-six individual episodes of conflict were collected in the two 12-week periods, with 34 (25%) being described as ongoing.
Data for the two data collection periods (2013 and 2014) were amalgamated after initial graphical display and showed no noteworthy differences between years.
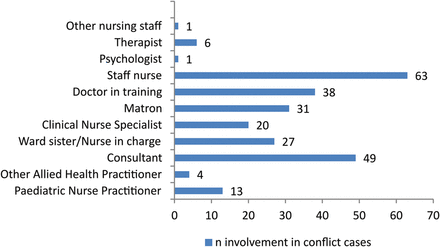
Figure 1 illustrates the number of staff experiencing conflicts, staff nurses, consultants, non-consultant doctors and matrons being involved most heavily. Forty-one per cent of conflicts were reported as having the involvement of only one healthcare professional and 33.6% involved two staff; the x axis of figure 1 therefore is staff involvement across all conflict cases (n=269) rather than the number of conflicts. There were only five reported incidents that involved more than five members of staff, representing less than 4% of all reported conflicts. There was a weak positive correlation (rs=0.26, n=134, p<0.001) of incidents which were rated as severe involving a larger number of healthcare professionals.
Staff involvement in conflicts experienced.
Consultants and senior nurses were often involved in managing conflict. Interviewees reported a dramatic impact of conflict on staff as individuals and as a functional clinical team:[Conflict will] distract attention from what really should be our clinical priority, which is looking after the seriously ill children, because everybody is caught up in the conflict situation. So, it has inappropriate demand and drain on the team, out of proportion to necessarily the medical issues of that particular child. So, it might take a registrar and an SHO and a consultant out of service for half a day dealing with a conflict situation (Consultant Paediatrician).
Staff time involved in conflict
A total of 448 h 45 min of healthcare professional time was taken up by these conflicts. Staff nurses, consultants and doctors in training were most heavily involved (n=133 cases; data on the staff and time involved in conflict were missing for three cases). On average, a conflict incident took up more than 3 h of staff time. Conflict incidences ranged in duration from 15 min to 56 h, and this was not normally distributed, with 72% of all incidents taking less than 180 min to resolve. The median duration was 82 min, and mode duration of 15 min. A moderate positive correlation was observed between rating of severity and time involved in conflict (rs=0.46, n=134, p<0.001), showing that more severe conflicts were associated with longer time taken to resolve the issue.
As can be seen in table 1, staff nurses and consultants spent the most time dealing with conflicts (113 h and 68 h 30 min, respectively). Further, some healthcare professional groups were never reported as having involvement in conflict (nursing assistants, therapy leads and Child and Adolescent Mental Health Service (CAMHS)) team).
Number of hours spent involved in conflict, stratified by profession
Severity
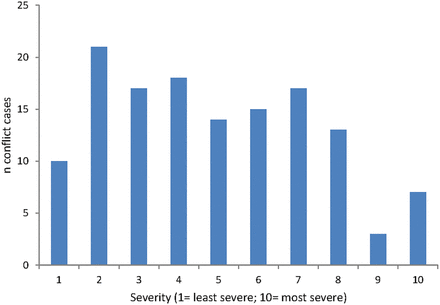
Severity was reported on a scale of 1 to 10, with 10 indicating most severe; mean severity was 4.9, with a SD of 2.5. The most frequently reported rating was 2 (15% of incidents being ranked as such) and the median score was 4.9. Figure 2 illustrates the spread of scores across the 135 cases where severity was recorded.
Severity scores for all cases.
Severity scores were designated into three groups: low (1–3), moderate (4–7) and high (8–10). Thirty-six per cent of all incidents were rated as low, 47% were rated as moderate and 17% were rated as high.
Qualitative interviews were used to aid interpretation of the numerical data. All interviewees defined the severity of conflict with reference to how easy and quick it would be to resolve. A score of 2–3 denoted a conflict which could be resolved in one discussion:A 2 or a 3 I think would be a little bit of conflict, a disagreement that is having an effect on the working of the ward so, it's slowing down the ward round, it's changing the order in which you have to see people there[…] you still have a working relationship, you're still able to move together and make a plan moving forward with the family there and in that terms of, you might agree to disagree, but actually you are still working together there, you reach a common goal there. (Registrar)
A score of 6–7 would require repeated conversations for resolution:[A 6 or 7 rating is] conflict that is manageable and doesn't end up completely derailing the treatment of the child, but which becomes really demanding. So, for example, you can have families who take an hour of the ward round time every day and then another member of the family comes in and you have to go through the whole thing again and lots and lots of explaining, lots and lots of questioning about why things are being done, child gets the treatment, everything eventually moves forward, but it is extremely demanding. (Consultant)
A score of 8–10 would necessitate security staff to keep staff safe and the patient ceasing to be the focus of conversations:8, 9 or 10, I would consider to be when I call security. So, violence and aggression, physical aggression. (Staff nurse)
Reasons for conflict
The three most common factors cited for the conflict across both years were ‘communication breakdown’, ‘disagreements about treatment’ and ‘unrealistic expectations’, as indicated in table 2. Respondents were able to identify multiple reasons for the conflict.
Reasons for conflict
Qualitative interviews examined the meaning attributed to the most frequent cause of conflict. ‘Communication breakdown’ was described as struggles in composing and decoding conversations about treatment choices which result in a lack of collaborative and joint understanding. Several interviewees felt that this was difficult to address, since most clinicians feel that they are good communicators:Communication breakdown, I would define it as the end point of efforts for one side or the other to get their point across and feeling it's not being heard in a way that they feel, they feel, they reach an impasse. (Paediatrician)
I actually don't think that necessarily everyone is good at communication, they think they are, but actually what you can visualise sometimes and see and witness, isn't always as good as they would like to perceive. (Senior nurse)
Twelve per cent of reasons were cited in the ‘other’ category. Of these 40 ‘other’ citations, 11 could be clustered under the umbrella ‘logistical issues’ in which difficulties or failures in organisation and scheduling of patients was a factor in conflict.
Location of conflict
The data were analysed to identify patterns of conflict frequency across wards/specialties. General paediatrics and the special care baby unit experienced the most severe conflicts, and neurology dealt with the greatest number of conflict incidents (see table 3; one case did not record specialty, n=135). Thirty-two per cent of the incidents reported within general paediatrics were rated as severe (ie, scored between 8 and 10).
Conflict incidence by specialty
Poor prognosis, complex multidisciplinary approaches and high levels of uncertainty were core themes identified by respondents to explain why neurology dealt with the highest number of conflicts:Children with neuro-disability and neurological problems are very difficult to manage, they have usually multi-system and multi-organ problems; it's very unusual for a child to just have a neurological problem. So, they may well have gastroenterology problems, they may well have respiratory problems and all sorts of other things so, they are complex children. I think the managing of[parental] expectations in neurology is extremely difficult because it's very difficult to prognosticate. (Consultant paediatrician)
We have a massive catchment area so, by the time you've got to us, you have often waited around for quite a while to get here, you have often been seen by professionals who have given or have been perceived to give bad advice because they're perceived to be not as expert. (Neurology registrar)
Discussion
Conflict was prevalent across paediatric specialties, with neurology dealing with the highest number of conflicts in the observed period. Nearly 450 h of healthcare practitioner time was taken over a 24-week period in managing conflict. Practitioners most commonly involved in conflicts were staff nurses, which may be explained by their frequent presence on wards throughout the day and night. The most commonly cited cause of conflict was communication breakdown.
The features cited as common to many intensive care settings are common to paediatric contexts.4 Advances in interventions have led to longer term survival of preterm infants and children with complex conditions but possibly also greater morbidity.26 The triadic dynamic of practitioner–parent–patient may increase the scope for conflict in decision-making, particularly around withholding or withdrawing life-sustaining treatment.5 Difficulties in accurate prognostication further exacerbate the scope for conflict.27
Conflict management is considered an important clinical competency for physicians.28–30 Strategies to reduce conflict would improve patient experience, support good working relationships31 and reduce the time and financial burden of conflict. Conflict reduction can be tackled through training,32 particularly in relation to communication since this is the area which is cited in most conflicts. Recently published guidelines assert that “all healthcare professionals should have access to continuing education in communication, ethics and law”5 indicating that communication training may complement other proposed interventions for managing conflict, such as decision-making tools.33 Focusing such interventions on front-line staff, notably staff nurses and consultant physicians is indicated by the data.
The data relied on healthcare staff reporting conflict, which introduces a number of potential biases and limitations; first staff needed to correctly identify conflict, and second, they then had to find the time to report it. Due to these limitations, it is likely conflicts were under-reported and the data reported here should be interpreted as a minimum. The scoring of conflict from 1 to 10 showed good consistency across the qualitative interviews; however, it is a limited scale. Development of a validated conflict scale in the healthcare setting would allow robust research and audit in conflict management. Further research questions could be asked of conflict occurrence, including the use of other methodologies to examine the minutia of such interactions, particularly where clinicians may report being good communicators. An approach such as conversation analysis would enable the identification of features of communication between clinicians and families where conflict is apparent34 leading potentially to new understandings and interventions. Our data include only staff rather than family reports of conflict, and consequently the data represent only a partial account of such incidences. Further work is required to fully understand parent/child experiences of conflict and to repeat this work in other paediatric settings to identify the extent to which services in other geographical and cultural contexts might differ in the incidence and severity of conflict experienced.
References
Footnotes
Twitter Follow Liz Forbat at @lizforbat
Contributors SB, LF and EM designed the work. CS and LF acquired the data. LF, CS, PM, EM and SB interpreted the data. LF, CS, EM and SB drafted the work and revised it critically for intellectual content. LF, CS, PM, EM and SB approved the final version of the manuscript. LF, PM, EM and CS agree to be accountable for all aspects of the work ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Funding The study was funded by the Guy's and St Thomas’ Charity. Grant: EFT120609.
Competing interests SB received a grant from the Guy's and St Thomas’ Charity during the conduct of the study; and she is the director of the Medical Mediation Foundation—an organisation which provides conflict management training and mediation in situations where there is disagreement/conflict between patients and healthcare professionals. However, the manuscript focuses on conflict incidence not mediation as a solution.
Provenance and peer review Not commissioned; internally peer reviewed.